Here is a number that should make you angry: medication non-adherence among seniors costs the American healthcare system over $528 billion every year. That is not a typo. Half a trillion dollars, gone. Not because the drugs do not work, but because the system that delivers them to real human beings is fundamentally broken.
And it gets worse. An estimated 125,000 people die in the United States each year because they did not take their medications correctly. Not because the prescription was wrong. Not because of some rare side effect. Because nobody was there to help them follow through. We spend billions developing the drugs, billions marketing them, billions getting them through FDA approval. Then we hand an 82-year-old woman a bag of seven different pill bottles with instructions printed in 8-point font and say good luck.
I have been thinking about this problem for a long time. Not as an abstract healthcare statistic, but as something I have watched happen in my own family. The confusion in my grandfather's eyes when he could not remember if he had already taken the morning round. My grandmother quietly skipping her blood pressure medication because it made her dizzy and she did not want to "bother" the doctor. These are not edge cases. This is the norm.
The Pill Organizer Is Not Going to Save Us
Let me describe the standard approach to medication adherence in this country. A doctor writes a prescription. The pharmacist fills it. Someone, maybe a nurse or a well-meaning family member, buys a plastic pill organizer with seven little compartments labeled Sunday through Saturday. Maybe there is a sticky note on the refrigerator. Maybe there is a phone alarm that goes off at 8 AM every day.
And then everyone walks away.
The pill organizer assumes the problem is remembering. So does the alarm. So does the app that sends push notifications to a phone your parent barely knows how to unlock. But remembering is only one piece of a much more complicated puzzle. Studies consistently show that fewer than half of seniors with chronic conditions take their medications as prescribed. Research from the World Health Organization puts average adherence for chronic illness at roughly 50% in developed nations. Fifty percent. Flip a coin. That is the current standard of care.
The apps are even worse. Most medication reminder apps have abandonment rates above 80% within the first month.
The people who need them most, seniors over 75 who manage multiple chronic conditions, are the least likely to use them consistently. You cannot solve a human problem with a notification badge.
Why People Actually Miss Their Medications
If you talk to geriatricians who spend their days with older patients, you hear the same stories over and over. The reasons seniors stop taking their medications are deeply human, and almost none of them have anything to do with forgetfulness.
- Complexity is the first culprit. The average American over 65 takes between four and five prescription medications daily. For those over 80, the number climbs to seven or more. Each one has different timing requirements. Some need food. Some forbid food. Some interact with each other in ways that were never explained clearly. When you are managing a regimen that complicated, missing one is not carelessness. It is probability.
- Then there is fear. Side effects that nobody warned them about, or that they were warned about but did not fully understand. The statin that makes their legs ache. The blood pressure pill that leaves them lightheaded every time they stand up. The diuretic that has them running to the bathroom every twenty minutes. Rather than calling the doctor and asking for an adjustment, many seniors simply stop taking the medication. They do not tell anyone. They just quietly put the bottle back in the cabinet.
- Depression plays a massive and underappreciated role. Research suggests that depressed patients are three times more likely to be non-adherent with their medications. And depression among seniors is staggeringly underdiagnosed. When you do not care whether you wake up tomorrow, taking a pill to lower your cholesterol feels pointless. The motivation to manage your health requires a basic belief that your health matters. Isolation erodes that belief faster than almost anything.
- And that brings us to the deepest root of the problem: loneliness. The US Surgeon General has compared the health effects of chronic loneliness to smoking 15 cigarettes a day. Research suggests that social isolation may increase dementia risk by as much as 31%. When someone lives alone and goes days without a meaningful conversation, medication adherence is just one of dozens of things that start to slip. It is a symptom, not the disease.
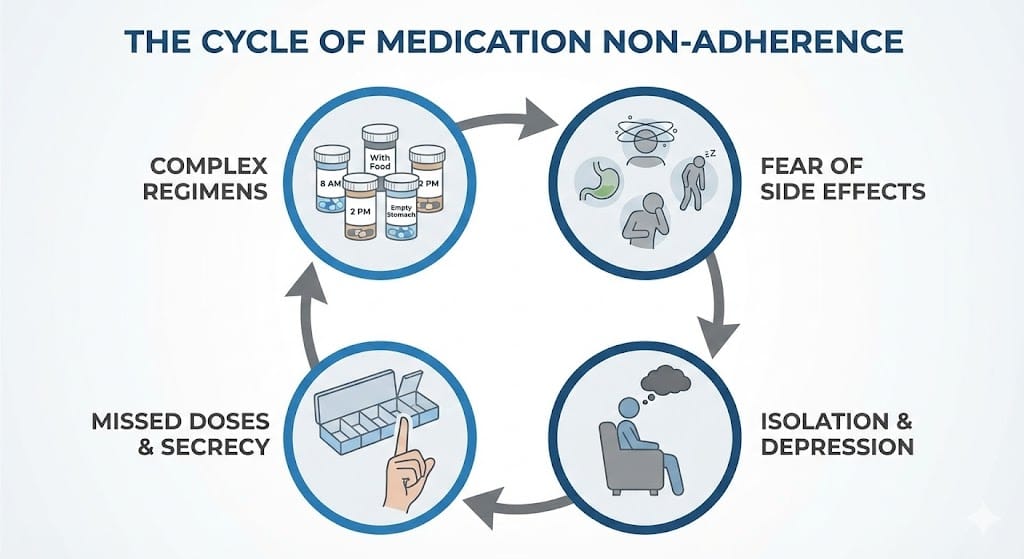
What a Conversation Can Catch That an Alarm Never Will
Think about the difference between a beep and a voice. An alarm goes off. You silence it. Maybe you take the pill, maybe you do not. There is no follow-up. No context. No one asking how you slept last night or whether your knee has been bothering you. No one noticing that you sound a little off today, a little more tired than usual, a little less engaged.
A daily phone conversation is a completely different thing. When someone calls and asks "Did you take your medications this morning?" as part of a genuine conversation about your day, something shifts. It is no longer a task on a checklist. It becomes part of a relationship. And relationships, more than any technology, are what drive behavior change.
But here is what most people miss: the real value of that conversation is not the reminder itself. It is everything else the conversation reveals.
When your parent mentions that the new pill makes them nauseous, that is critical information a doctor needs to hear. When they casually say they have not been eating much this week, that is a red flag. When they cannot remember what day it is, that is a data point that might not show up at a scheduled appointment for another three months.
Daily reminders can increase medication adherence up to 90% when they are embedded in actual human interaction rather than automated notifications. That number comes not from a clever app interface but from the simple power of someone consistently showing up and asking.
Building Something That Actually Works
So what does an effective medication adherence system look like for seniors? Not the theoretical kind that works in a clinical trial with motivated, supervised participants. The real kind that works for an 84-year-old woman living alone in a two-bedroom apartment in Sacramento who has mild cognitive impairment and whose kids live three states away.
It needs three layers.
- A consistent daily touchpoint. Not an alarm. Not a text message. A voice. Someone or something that calls at the same time every day and asks how they are doing, checks on their medication, and actually listens to the answer. This is what services like VoiceLegacy's daily companion calls are built to do. No app to download, no device to set up. Just a phone call on any phone, including a landline.
- It needs intelligent escalation. When something seems off, when someone mentions they stopped taking a medication or sounds confused about their regimen, that information has to go somewhere useful. Not into a database that nobody checks. To a caregiver, a family member, or a healthcare provider who can actually intervene. This is the gap that smart triage and alert systems are designed to fill. Pattern recognition across daily interactions surfaces problems early, before they become emergencies.
- This is the part that almost everyone overlooks, it needs to address the emotional infrastructure underneath the adherence problem. A person who feels connected, who has something to look forward to each day, who believes their health matters to someone, is a person who takes their medications. This is not soft science. This is the mechanism. Early research suggests that consistent social interaction may reduce depression symptoms by as much as 51%. When depression lifts, adherence follows.
The Prescription Nobody Writes
There is something almost absurd about the current state of affairs. We have a healthcare system that will spend $300,000 on a hospitalization caused by medication non-adherence but will not spend $50 a month on daily check-in calls that could have prevented it.
We will write a prescription for a drug that costs $400 a month but not for the conversation that makes someone actually take it.
I keep thinking about something a geriatrician told me years ago. She said the most powerful intervention she had ever seen for medication adherence was not a new drug, not a better pill organizer, not a smart pill bottle with Bluetooth. It was a granddaughter who called every morning at 7:30 and said, "Nana, did you take your pills?" That is it. That was the whole intervention. And it worked better than anything else she had tried in thirty years of practice.
The problem, of course, is that not every senior has a granddaughter who can call at 7:30 every morning. Not every family lives close enough, has the bandwidth, or even knows there is a problem. Sixty percent of nursing home residents receive no regular visitors at all. For the 14 million Americans over 65 who live alone, the gap between what they need and what they get is enormous.
That gap does not have to stay open. The technology exists today to provide daily, personalized, conversational check-ins that include medication reminders as part of a broader wellness conversation. It works on any phone. It remembers what medications someone takes and when. It notices when patterns change. And most importantly, it gives someone a reason to pick up the phone.
We do not have a pill problem in this country. We have a people problem. We hand seniors the medications they need and then leave them alone to figure it out. And when they fail, we blame them for being forgetful, non-compliant, difficult. We invented a clinical term for it. Non-adherence. As if the problem is the patient.
The problem is not the patient. The problem is the silence between prescriptions. It is the empty kitchen at 8 AM when the pills are sitting on the counter and nobody is there to say, "Good morning. How are you feeling? Did you take your medication today?" Fill that silence, and you will solve more than medication adherence. You will solve something much bigger.
If you have a parent or grandparent managing medications alone, call them today. Not to lecture. Not to organize their pills. Just to talk. Ask how they are feeling. Ask if anything has changed. Ask if the new medication is working. You might be surprised by what you hear. And you might be the reason they take their pills tomorrow morning.

Written by
Sihwa Jang
